Specialized Advanced Dentistry,
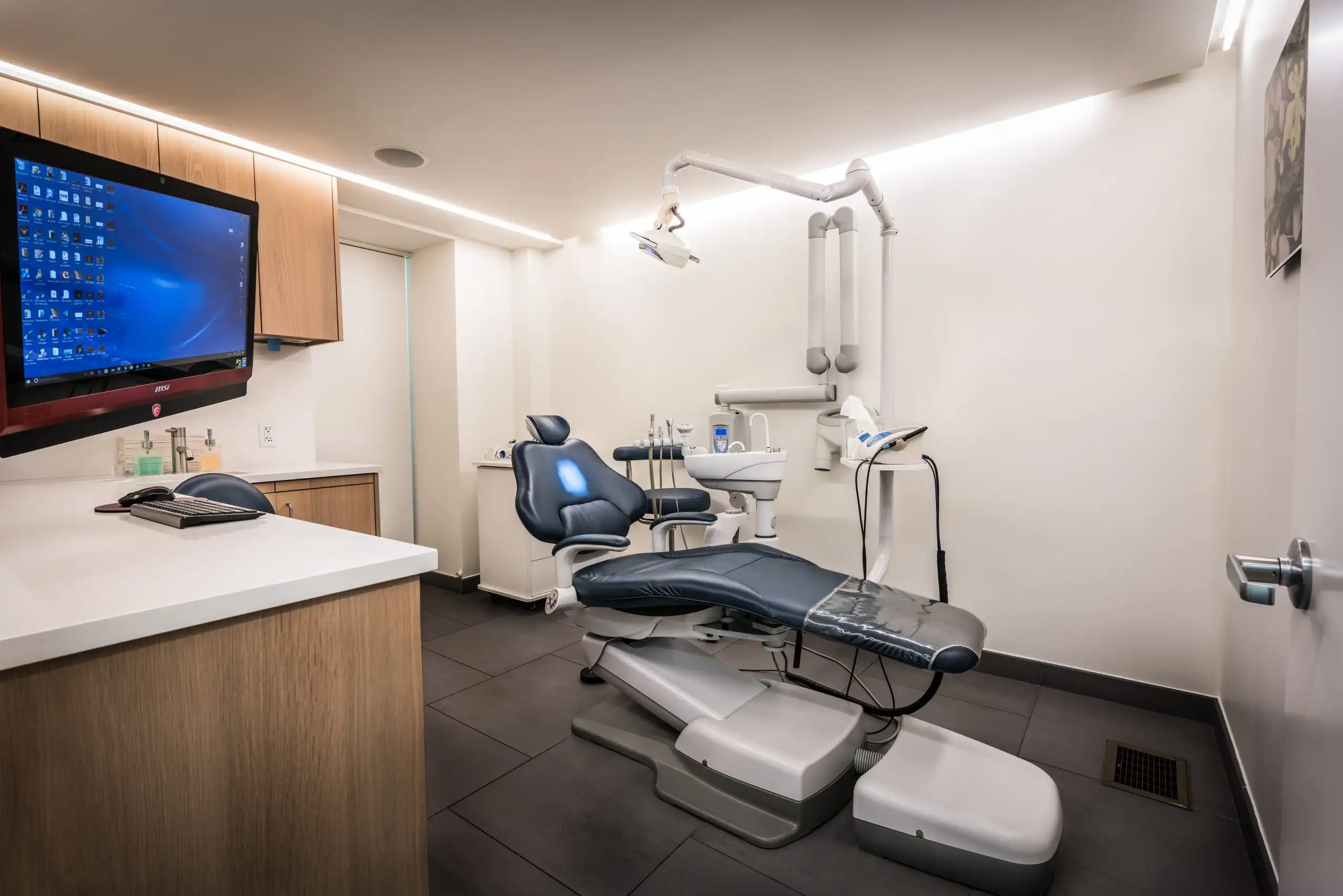
State of the Art Technologies.
We are proud to offer our patients the most personalized and advanced dental care. The experience and commitment of our practice is unique combining science and artistry for a healthy smile.
OUR DENTAL SERVICES
We provide patients with the best solutions to improve and maintain a healthy smile.
Your bone and gum tissue should fit snugly around your teeth like a turtleneck around your neck. When you have periodontal disease, this supporting tissue and bone is destroyed, forming "pockets" around the teeth.
Over time, these pockets become deeper, providing a larger space for bacteria to live. As bacteria develop around the teeth, they can accumulate and advance under the gum tissue. These deep pockets collect even more bacteria, resulting in further bone and tissue loss. Eventually, if too much bone is lost, the teeth will need to be extracted.
Your periodontist has measured the depth of your pocket(s). A periodontal pocket reduction procedure has been recommended because you have pockets that are too deep to clean with daily at-home oral hygiene and a professional care routine.
During this procedure, your periodontist folds back the gum tissue and removes the disease-causing bacteria before securing the tissue into place. In some cases, irregular surfaces of the damaged bone are smoothed to limit areas where disease-causing bacteria can hide. This allows the gum tissue to better reattach to healthy bone.
Reducing pocket depth and eliminating existing bacteria are important to prevent damage caused by the progression of periodontal disease and to help you maintain a healthy smile. Eliminating bacteria alone may not be sufficient to prevent disease recurrence. Deeper pockets are more difficult for you and your dental care professional to clean, so it's important for you to reduce them. Reduced pockets and a combination of daily oral hygiene and professional maintenance care increase your chances of keeping your natural teeth – and decrease the chance of serious health problems associated with periodontal disease.
Oral medicine is concerned with clinical diagnosis and non-surgical management of non-dental pathologies affecting the orofacial region (the mouth and the lower face). Many systemic diseases have signs or symptoms that manifest in the orofacial region. Pathologically, the mouth may be afflicted by many cutaneous and gastrointestinal conditions. There is also the unique situation of hard tissues penetrating the epithelial continuity (hair and nails are intra-epithelial tissues). The biofilm that covers teeth therefore causes unique pathologic entities known as plaque-induced diseases.
Example conditions that oral medicine is concerned with are lichen planus and pemphigus vulgaris. Moreover, it involves the diagnosis and follow-up of pre-malignant lesions of the oral cavity, such as leukoplakias or erythroplakias and of chronic and acute pain conditions such as paroxysmal neuralgias, continuous neuralgias, myofascial pain, atypical facial pain, autonomic cephalalgias, headaches and migraines. Another aspect of the field is managing the dental and oral condition of medically compromised patients such as cancer patients suffering from related oral mucositis, bisphosphonate-related osteonecrosis of the jaws or oral pathology related to radiation therapy. To get a definitive diagnosis, most of the time, we will perform a surgical excisional biopsy and send to a pathology lab. The results will be communicated with you. If further treatment or referral is needed, out periodontist will guide in that process.
A key to implant success is the quantity and quality of the bone where the implant is to be placed. The upper back jaw has traditionally been one of the most difficult areas to successfully place dental implants due to insufficient bone quantity and quality and the close proximity to the sinus. If you've lost bone in that area due to reasons such as periodontal disease or tooth loss, you may be left without enough bone to place implants.
Sinus lift surgery can help correct this problem by raising the sinus floor and developing bone for the placement of dental implants. Several techniques can be used to raise the sinus and allow for new bone to form. In one common technique, an incision is made to expose the bone. Then a small circle is cut into the bone. This bony piece is lifted into the sinus cavity, much like a trap door, or removed during the preparation, and the space underneath is filled with bone graft material. Your periodontist can explain your options for graft materials, which can regenerate lost bone and tissue.
Finally, the incision is closed and healing is allowed to take place. Depending on your individual needs, the bone usually will be allowed to develop for about four to 12 months before implants can be placed. After the implants are placed, an additional healing period is required. In some cases, the implant can be placed at the same time the sinus is augmented.
Undergoing sinus lift surgery has been shown to greatly increase your chances for successful implants that can last for years to come. Many patients experience minimal discomfort during this procedure.
Scaling and root planning is a careful cleaning of the root surfaces to remove plaque and calculus [tartar] from deep periodontal pockets and to smooth the tooth root to remove bacterial toxins using hand instruments. Scaling and root planing is sometimes followed by adjunctive therapy such as local delivery antimicrobials, systemic antibiotics, and host modulation, as needed on a case-by-case basis. This in the old conventional used to be only with hand instruments. With new advent modality of treatment, it appears that the laser was able to provide better accessibility, removal of the infected inner covering of the periodontal pocket and creates blood clot essential point in wound healing. This will be followed by a phase of re-evaluation. Some patients will not require any further active treatment and some will require surgical corrective therapy. However, the majority of patients will require ongoing maintenance therapy to sustain health.
Commonly known as root canal, is a treatment sequence for the infected pulp (nerve) of a tooth which is intended to result in the elimination of infection and the protection of the decontaminated tooth from future microbial invasion. Root canals and their associated pulp chamber, are the physical hollows within a tooth that are naturally inhabited by nerve tissue, blood vessels and other cellular entities. Together, these items constitute the dental pulp.
Endodontic therapy involves the removal of these structures, disinfection and the subsequent shaping, cleaning, and decontamination of the hollows with small files and irrigating solutions, and the obturation (filling) of the decontaminated canals. Filling of the cleaned and decontaminated canals is done with an inert filling such as gutta-percha and typically a Zinc oxide eugenol-based cement to bind gutta-percha in some root canal procedures.
A dental implant is an artificial tooth root that is placed into your jaw to hold a replacement tooth or bridge. Dental implants may be an option for people who have lost a tooth or teeth due to periodontal disease, an injury, or some other reason. This type of implant is generally used as an alternative for patients with bridges or removable dentures. There are two types titanium and ceramics. The latter is a new addition but without a long term studies to support its success. If you have concerns of metal and you request a ceramic implant, we are providing it in our practice. They are all screw type devices placed in the bone. Each implant holds one or more prosthetic teeth.
Read moreDeformities in the upper or lower jaw can leave you with inadequate bone in which to place dental implants. This defect may have been caused by periodontal disease, wearing dentures, developmental defects, injury or trauma. Not only does this deformity cause problems in placing the implant, it can also cause an unattractive indentation in the jaw line near the missing teeth that may be difficult to clean and maintain.
To correct the problem, the gum is lifted away from the ridge to expose the bony defect. The defect is then filled with bone or bone substitute to build up the ridge. Your periodontist can tell you about your options for graft materials, which can help to regenerate lost bone and tissue.
Finally, the incision is closed and healing is allowed to take place. Depending on your individual needs, the bone usually will be allowed to develop for about four to 12 months before implants can be placed. In some cases, the implant can be placed at the same time the ridge is modified.
Ridge modification has been shown to greatly improve appearance and increase your chances for successful implants that can last for years to come. Ridge modification can enhance your restorative success both aesthetically and functionally.
Periodontists are often considered the plastic surgeons of dentistry. If you are looking to improve your smile, a periodontist may be able to help.
Gummy smile or uneven gum line.Do you feel your teeth look too short and your smile is too gummy or your gums cover too much of some teeth while leaving the others the right length? If so, dental crown lengthening might be the solution for you. During this procedure, excess gum tissue is removed to expose more of the crown of the tooth. Then your gumline is sculpted to give your new smile just the right look.
Long teeth / exposed roots.ometimes gum recession causes the tooth root to become exposed, which makes your teeth look long and can make you look older than you are. This recession can happen as a result of a variety of causes, including periodontal diseases. Gum graft surgery and other root coverage procedures are designed to cover exposed roots, to reduce further gum recession and to protect vulnerable roots from decay.
Indentations in the gums and jawbone.Tooth loss can cause an indentation in the gums and jawbone where the tooth used to be. This happens because the jawbone recedes when it no longer is holding a tooth in place. Not only is this indention unnatural looking, it also causes the replacement tooth to look too long compared to the adjacent teeth. Ridge augmentation can fill in this defect recapturing the natural contour of the gums and jaw. A new tooth can then be created that is natural looking, easy to clean and beautiful.
Procedures that regenerate lost bone and tissue supporting your teeth can reverse some of the damage caused by periodontal disease. Your periodontist may recommend a regenerative procedure when the bone supporting your teeth has been destroyed due to periodontal disease. These procedures can reverse some of the damage by regenerating lost bone and tissue.
During this procedure, your periodontist folds back the gum tissue and removes the disease-causing bacteria. Membranes (filters), bone grafts or tissue-stimulating proteins can be used to encourage your body's natural ability to regenerate bone and tissue. Eliminating existing bacteria and regenerating bone and tissue helps to reduce pocket depth and repair damage caused by the progression of periodontal disease. With a combination of daily oral hygiene and professional maintenance care, you'll increase the chances of keeping your natural teeth – and decrease the chances of other health problems associated with periodontal disease.
Exposed tooth roots are the result of gum recession. Gum graft surgery will repair the defect and help to prevent additional recession and bone loss. Gum grafts can be used to cover roots or develop gum tissue where absent due to excessive gingival recession. During gum graft surgery, your periodontist takes gum tissue from your palate or another donor source to cover the exposed root. This can be done for one tooth or several teeth to even your gum line and reduce sensitivity.
What are the benefits of gum graft surgery?A gum graft can reduce further recession and bone loss. In some cases, it can cover exposed roots to protect them from decay. This may reduce tooth sensitivity and improve esthetics of your smile. Whether you have a gum graft to improve function or esthetics, patients often receive the benefits of both: a beautiful new smile and improved periodontal health – your keys to smiling, eating and speaking with comfort and confidence.
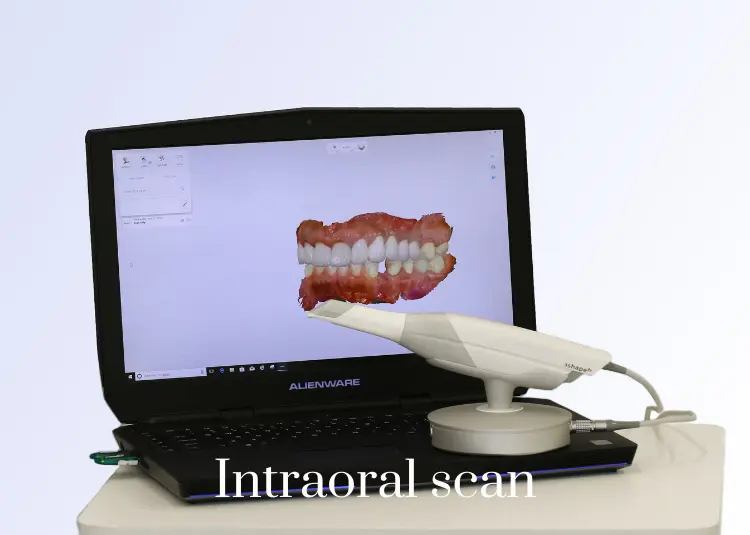
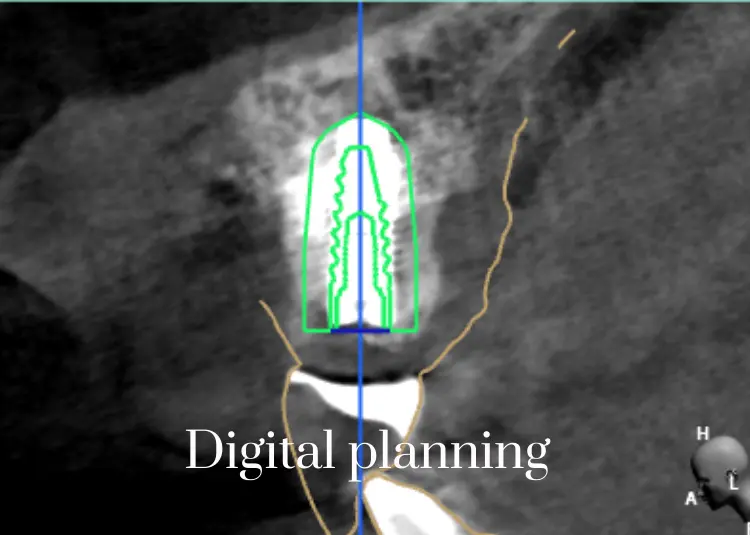
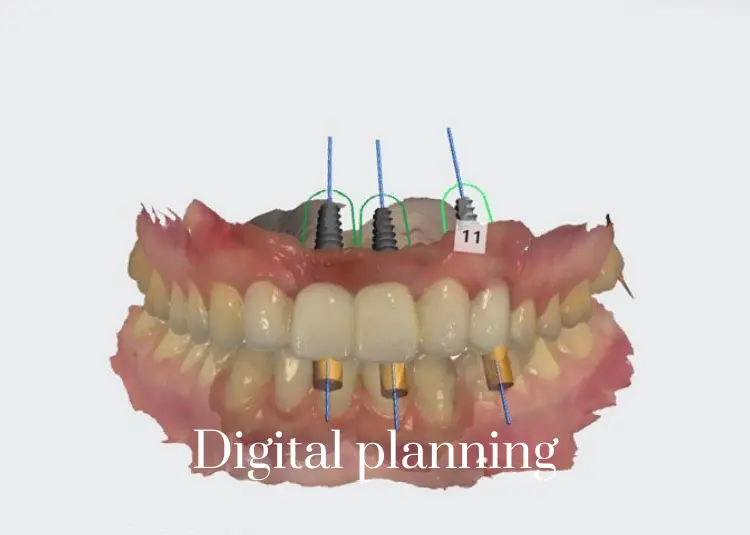
Digital Dentistry has changed treatment planning. Using this new technology, your case is virtually planned and ready for execution. With digital scanning, we have eliminated dental impression material and increased the accuracy of our final dental product. As always, our goal is to give you the best, most innovative service and we are keeping our promise.
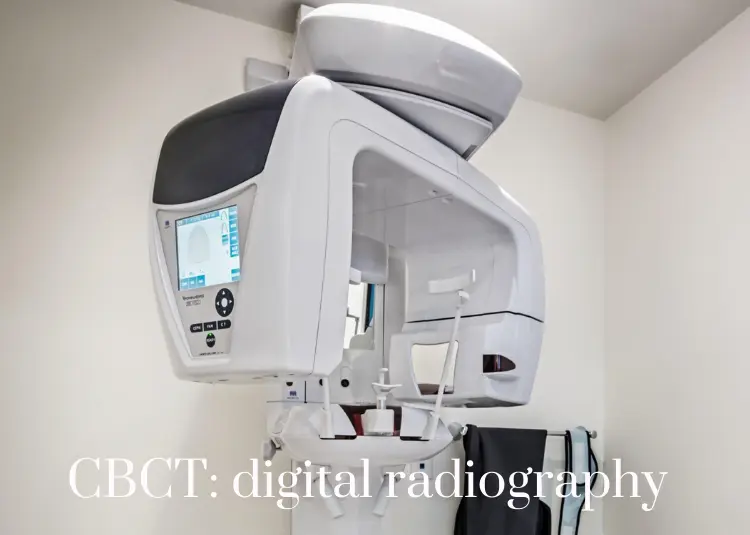
The term All-on-4 refers to "all" teeth being supported "on four" dental implants. This procedure allow the replacement of missing teeth with a permanent, screw-retained, same-day replacement for the entire upper and / or lower set of teeth with a bridge or denture. The procedure is best for patients with significant tooth loss or decay and for people whose bone loss in the jaw area prevents them from getting conventionally oriented (vertical) dental implants. Often, tooth loss is accompanied by loss of the jaw bone which poses the problem of reconstruction of the jaw bone requiring bone grafting. The All-on-4 technique takes advantage of the dense bone that remains in the front part of the jaws and by placing the two posterior implants on an angle to avoid the sinus cavities in the upper jaw and the nerve canal in the lower jaw. For the implementation to be successful a careful analysis of the bone structure needs to be made. The most ideal way to evaluate the bone is by a CBCT scan and digital planning. The All-on-4 protocol is for at least four implants to be placed in a jaw. The back implants are typically angled approximately 30 to 45 degrees from the biting plane. The implant is placed in front of the maxillary sinus in the upper jaw (maxilla) and in front of the mental nerve in the lower jaw (mandible). The head of the implant emerges in approximately the second premolar position. This will allow a molar tooth to be cantilevered posterior resulting in a denture or bridge with approximately 12 teeth.
Known as Socket preservation or alveolar ridge preservation procedure. It allows to reduce bone loss after tooth extraction. After tooth extraction, the jaw bone has a natural tendency to lose its original width resulting in 30–60% loss in bone volume in the first six months. Bone loss, can compromise the ability to place a dental implant (to replace the tooth), its aesthetics and functional ability.
A 2015 Cochrane study found that there was evidence that socket preservation does indeed improve the height and width, compared to extraction without socket preservation but that there is insufficient data to conclude that it decreases implant failures, improves aesthetics, or that one grafting material is any better than another.
Socket preservation is completed at the time of extraction. After removal of the tooth, the gum is elevated away from the bone if needed, the socket is thoroughly cleansed mechanicaaly with curettes and chemically and than thoroughly rinsed with saline (sterile) water. The socket is packed with bone grafting material and a resorbable collagen barrier membrane is placed over the graft. The wound will be closed over the barrier membrane.
The procedure of placing dental implants is to replace damaged or missing teeth (i.e., bad teeth) with artificial teeth that function and appear like a real tooth. Dental implants offer an alternative to dentures or bridgework that may not always fit as well in the patient's mouth. Dental implants are surgically placed in your jawbone and serve as the roots of missing bad teeth.
Over the last decade or so there has been a great interest in atraumatic extractions, which is attributable largely to the desire for dentists wanting to do immediate dental implant placement. Atraumatic extractions are desired more and more to preserve bone for immediate implant placement. In general, the benefit of dental implants is solid support for the patient's new teeth, which requires the bone around the dental implant to heal. Depending on how the tooth extraction is performed, the healing time required can vary greatly, hence the desire to perform an atraumatic extraction.
An increasingly common strategy to preserve bone and reduce treatment times includes the placement of a dental implant into a recent tooth extraction site. Also, immediate loading is becoming more common as success rates for this procedure are much more acceptable. Immediate placement can eliminate months off treatment time and in some cases a prosthetic temporary tooth can be attached to the tooth implants at the same time as the surgery to place the dental implants. There is data that suggests when placed into a single rooted tooth sites with healthy bone and mucosa around them, the success rates are generally comparable to that of delayed procedures with no additional complications.
The advantageous of such procedure are numerous, but we will emphasis on the aesthetic preservation, shortening the time for the patient to receive a final prosthetic restoration and the cost of site preservation.
A key to implant success is the quantity and quality of the bone where the implant is to be placed. The upper back jaw has traditionally been one of the most difficult areas to successfully place dental implants due to insufficient bone quantity and quality and the close proximity to the sinus. If you've lost bone in that area due to reasons such as periodontal disease or tooth loss, you may be left without enough bone to place implants.
If you have a minimum of 4 mm below the sinus, at the time of the implant placement preparation, tools can be used to infract the floor of the sinus and the bone graft is pushed to increase the length and surround the implant with bone. It will be left to heal up to 6 months and after that the implant will be uncovered if it was buried under the gum to attach an extension. This temporary healing cap completes the foundation on which your new tooth will be placed. Your gums will be allowed to heal for a couple of weeks following this procedure and then your dentist will proceed with restoring the implant and place the dental prosthetic engaged to that implant.
Invisalign treatment is the process of wearing a series of clear, removable aligners that gradually straighten your teeth. No brackets and wires, and none of the restrictions that come with metal braces.
The purpose is to remove an infection in the periradicular tissue around a root canal treated tooth, which is impeding the healing of the tooth after conventional root canal treatment. After removing the pulp, the aim of endodontic treatment is to seal the pulpal space to prevent further bacterial contamination and allow healing of the periradicular tissue. Success rates for root-canal treatment range from 47 to 97 percent; failures may be due to spaces in the root-canal filling, a root filling which is too short or a preexisting periapical lesion.
Works by inhibiting the intensity of the contraction of jaw muscles. This can last up to three months and has multiple dental applications such as; treatment of Temporomandibular Joint Disorder which is associated with jaw pain, facial pain and headaches, relief of clenching and tooth grinding, slenderizing enlarged jaw muscles (Masseter hypertrophy ), and migraine headache relief.
Botox CosmeticWorks by temporarily inhibiting the intensity of the contraction of facial muscles to smooth out wrinkles on the forehead, around the eyes and mouth, treating gummy smiles by dropping the lip or treating asymmetric smiles due to uneven contraction.
Dermal Fillers(Hyaluronic acid which is naturally present in 56% of body tissue) can be used in the peri-oral area to enhance a smile by restoring volume to the lips and face. Hyaluronic acid can stimulate fibroblast cells in the skin to produce new collagen, and help to fight wrinkles rather than just fill them. Dermal fillers can last from 4 months to one year. Repeated treatment encourages collagen to grow and maintain the results longer. Commonly treated areas are lip enhancement, nasolabial folds ( the parentheses around the mouth ), marionette lines, pre-jowl sulcus, and smokers' lines.
A gum graft (also known as a gingival graft or periodontal plastic surgery), is a collective name for many different surgical periodontal procedures that aim to cover an exposed tooth root surface with grafted oral tissue.
Exposed tooth roots are usually the result of gingival recession due to periodontal disease. There are other common causes, including overly aggressive brushing and trauma. FREE GINGIVAL GRAFT PROCEDURESubepithelial connective tissue graft
In 2015 the American Academy of Periodontology Regeneration Workshop concluded that this procedure (SCTG) is considered the "gold standard" for treating gum recession due to it's long lasting and well documented success rate (more than 30 years). Tissue is removed fairly painlessly from the inner layer of the palate and relocated to the site of gum recession. The advantages are that the tissue becomes thicker, matches the adjacent tissue in texture and color and has initial healing in one week. (See examples below)
Acellular dermal matrix allograftThis procedure uses medically processed, donated human tissue as a tissue source for the graft. The advantage of this is procedure is that there is no need for a donor site from the patient’s palate (and thus, less pain).
Chao Pinhole® Surgical TechniqueThis procedure is performed by making small holes with a needle in the gum tissue. Using specially designed instruments, the gum tissue is loosened and guided over the receded part of the tooth. No palatal donor tissue is necessary.

Accepted methods of payment
Cash, Debit, Credit Cards Personal Checks Third Party Financing – CareCredit In-office payment plans - Payments can be split in three payments after 25% deposit at the time of the scheduling appointment.